Overview
Ventricular repair, or cardiorrhaphy, has long been one of the most dramatic and lifesaving procedures performed in the emergency department. Around 3000 BC, in the Edwin Smith Surgical Papyrus, the first reports of trauma to the thorax were described.
Ventricular repair, or cardiorrhaphy, has long been one of the most dramatic and lifesaving procedures performed in the emergency department. Around 3000 BC, in the Edwin Smith Surgical Papyrus, the first reports of trauma to the thorax were described.
The first successful human cardiorrhaphy was performed by German physician Rehn in 1896 to repair a right ventricular injury sustained during a fencing match. The first successful cardiorrhaphy in the United States was performed by Hill in 1902; he operated on a teenage stabbing victim on a kitchen table in Montgomery, Alabama. This began the practice of emergent cardiac repair in patients who sustain life-threatening penetrating trauma to the heart.
Cardiac trauma is divided into 2 mechanisms: blunt and penetrating.
- Blunt injuries: Cardiac rupture following blunt thoracic trauma usually causes death at the scene and is not typically encountered clinically.
- Penetrating injuries: These are also commonly lethal but can be salvageable. The most common causes of death from penetrating trauma wounds are cardiac tamponade and exsanguination. In contradistinction to other forms of trauma, preoperative resuscitation plays a limited role, and immediate surgical intervention is a superior determinant of survival.
Consider cardiac injury in the differential whenever penetrating injury has occurred in the thorax or upper abdomen. The area of most concern is known as the cardiac box. This is an area of the trunk in which penetrating injuries risk damage to the heart. Anatomically, this is a triangular region bordered by the midclavicular lines laterally, the clavicles superiorly, and the costal margins inferiorly.
Clinical presentations can vary widely, from hemodynamically stable to cardiac arrest. Cardiac tamponade is commonly thought to correlate with the Beck triad (hypotension, elevated jugular venous pressure, and muffled heart sounds), but these symptoms are found only in a minority of patients. Signs of shock (eg, tachycardia, hypotension, diaphoresis, and agitation) are better correlated with tamponade and should, therefore, be assessed.
The chest radiograph does not commonly show an enlarged cardiac silhouette, even in the setting of acute tamponade. In cases of suspected penetrating cardiac injury, radiography should be used to assess for clues of cardiac injury, including retained intracardiac foreign bodies, hemothorax, pneumothorax, or pneumoperitoneum. For more information, see Medscape Reference article Pneumothorax Imaging. See the image below.
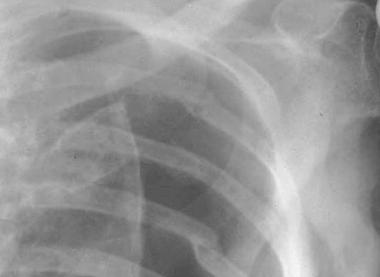
The Focused Assessment with Sonography in Trauma (FAST) examination is rapidly becoming the diagnostic tool of choice in the emergency department for identifying pericardial effusions. It does have its limitations, however, as it is both operator- and patient-dependent. It should be used primarily to direct and prioritize management.
An essential part of the management of patients in extremis from cardiac injury is thoracotomy for cardiac resuscitation, and possible cardiorrhaphy. The thoracotomy involves making a large incision to expose the heart, aorta and hilum. It allows for internal defibrillation and cardiac massage. Once the heart is exposed, a pericardial incision can be made to release any tamponade. The heart is then examined to look for any penetrating wounds. For a detailed description of this procedure, see Medscape Reference article Emergency Bedside Thoracotomy.
Multiple methods are used in the emergent management of cardiac wounds.
-
Digital pressure: This method is used for small wounds and can be used to control bleeding on the way to the operating room.
-
Foley catheter: For larger wounds, a Foley catheter can be inserted through the wound and inflated; with gentle traction, tamponade can be accomplished. Placing a Foley catheter can also stop hemorrhage so cardiorrhaphy can be performed or so a patient can be transported to the operating room for repair. An additional advantage of using the Foley catheter is the ability to administer intracardiac medications, fluids, or blood.
- Immediate cardiorrhaphy (in the emergency department): This method has been found to yield a survival rate up to 31% in patients presenting with penetrating cardiac injuries.
Indications
The science of surgical resuscitation has advanced tremendously since Rehn performed the first human cardiorrhaphy. The popularity of this procedure has waxed and waned as a result of changes in surgical techniques and differing analyses of patient outcome data. Currently, the indications for emergent thoracotomy, with or without cardiorrhaphy, include the following:
-
Persistent hypotension or signs of cardiac tamponade in the setting of penetrating chest trauma
-
Cardiac arrest in the emergency department, in the setting of blunt trauma
Contraindications
See the list below:
-
Clinically stable patient
-
Patient with evidence of prolonged death (eg, rigor mortis, livor mortis)
-
Patient whose life is unsalvageable (eg, decapitation)
Anesthesia
See the list below:
-
Always attend to the ABCs (airway, breathing, circulation), particularly in trauma patients. Ideally, intubate patients prior to thoracotomy or cardiorrhaphy. If that is not possible, intubate during the procedure. Administer general anesthesia using rapid sequence intubation protocols and postintubation sedation, analgesia, or paralysis. For more information, seeTracheal Intubation, Rapid Sequence Intubation and Tracheal Intubation, Medications.
-
Local anesthesia is not feasible and may cause life-threatening arrhythmias, as the maximum dose of lidocaine may be exceeded for a thoracotomy incision. Observe the patient for signs of pain or agitation (eg, tachycardia or tachypnea). Choose appropriate sedative and neuromuscular blocking agents to maintain both cardiovascular output and effective anesthesia
Equipment
The thoracotomy tray should include the following:
-
Sterile preparatory tray
-
Scalpel, No. 10 or No. 20
-
Mayo or Metzenbaum scissors
-
Rib spreader
-
Tissue forceps, 2
-
Satinsky vascular clamps, 2
-
Lebsche knife
-
Hegar needle holders, 3
-
Nylon (3-0) or Prolene (2-0) suture on a curved needle
-
Teflon pledgets
-
Suture scissors
-
Surgical stapler
-
Sterile towels
-
Sponges
-
Foley catheter
-
Chest tube
-
Towel clips
Positioning
See the list below:
-
Place the patient in a supine position with the left anterior chest wall exposed.
-
Place the patient’s left arm above the head, and place a rolled towel or sheet under the left side for optimal exposure and to ensure a wide incision.
-
Prepare the left anterior chest wall with povidone-iodine (Betadine) solution and sterile towels. Note, however, that preprocedural antiseptic skin preparation may be ineffective and may delay the procedure
Soure emedicine.com
Duc Tin Surgical Clinic
Tin tức liên quan
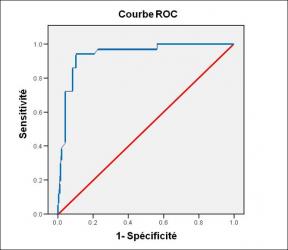
Performance diagnostique de l’interféron gamma dans l’identification de l’origine tuberculeuse des pleurésies exsudatives
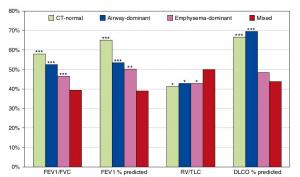
A Mixed Phenotype of Airway Wall Thickening and Emphysema Is Associated with Dyspnea and Hospitalization for Chronic Obstructive Pulmonary Disease.
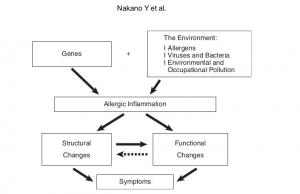
Radiological Approach to Asthma and COPD-The Role of Computed Tomography.

Significant annual cost savings found with UrgoStart in UK and Germany
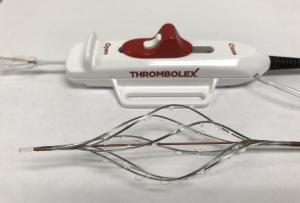
Thrombolex announces 510(k) clearance of Bashir catheter systems for thromboembolic disorders
Phone: (028) 3981 2678
Mobile: 0903 839 878 - 0909 384 389