Cardiac markers are used in the diagnosis and risk stratification of patients with chest pain and suspected acute coronary syndrome (ACS). The cardiac troponins, in particular, have become the cardiac markers of choice for patients with ACS.
Indeed, cardiac troponin is central to the definition of acute myocardial infarction (MI) in the consensus guidelines from the European Society of Cardiology (ESC) and the American College of Cardiology (ACC): These guidelines recommend that cardiac biomarkers should be measured at presentation in patients with suspected MI, and that the only biomarker that is recommended to be used for the diagnosis of acute MI at this time is cardiac troponin due to its superior sensitivity and accuracy.
For example, patients with elevated troponin levels but negative creatine kinase-MB (CK-MB) values who were formerly diagnosed with unstable angina or minor myocardial injury are now reclassified as non–ST-segment elevation MI (NSTEMI), even in the absence of diagnostic electrocardiogram (ECG) changes.
Similarly, only 1 elevated troponin level above the established cutoff is required to establish the diagnosis of acute MI, according to the ACC guidelines for NSTEMI.
These changes were instituted following the introduction of increasingly sensitive and precise troponin assays. Up to 80% of patients with acute MI will have an elevated troponin level within 2-3 hours of emergency department (ED) arrival, versus 6-9 hours or more with CK-MB and other cardiac markers.
Accordingly, some have advocated relying solely on troponin and discontinuing the use of CK-MB and other markers. [7, 8, 9, 10, 11] Nevertheless, CK-MB and other markers continue to be used in some hospitals to rule out MI and to monitor for additional cardiac muscle injury over time.
Note that cardiac markers are not necessary for the diagnosis of patients who present with ischemic chest pain and diagnostic ECGs with ST-segment elevation. These patients may be candidates for thrombolytic therapy or primary angioplasty. Treatment should not be delayed to wait for cardiac marker results, especially since the sensitivity is low in the first 6 hours after symptom onset. ACC/American Heart Association (AHA) guidelines recommend immediate reperfusion therapy for qualifying patients with ST-segment elevation MI (STEMI), without waiting for cardiac marker results.
Cardiac Troponins
The troponins are regulatory proteins found in skeletal and cardiac muscle. Three subunits have been identified: troponin I (TnI), troponin T (TnT), and troponin C (TnC). The genes that encode for the skeletal and cardiac isoforms of TnC are identical; thus, no structural difference exists between them. However, the skeletal and cardiac subforms for TnI and troponin TnT are distinct, and immunoassays have been designed to differentiate between them.
Two different reference ranges are used in troponin assays. The upper percentile reference limit gives the upper limit of what can be expected in a normal, healthy, adult population, while the coefficient of variation (CV) is the percent variation in assay results that can be expected when the same sample is repeatedly analyzed.
According to European Society of Cardiology (ESC)/American College of Cardiology Foundation (ACCF)/American Heart Association (AHA)/ World Heart Federation (WHF) guidelines, MI refers specifically to myocardial necrosis due to myocardial ischemia. However, although elevations in the serum levels of TnI, TnT, and CK-MB indicate the presence of injury-associated necrosis of myocardial cells, such elevations do not point to the underlying mechanism of the necrosis. While myocardial necrosis occurs in MI, it can also be a product of predominantly nonischemic myocardial injury, as occurs in association with heart failure, arrhythmia, myocarditis, renal failure, pulmonary embolism, and percutaneous or surgical coronary procedures.
The sensitivity, specificity, and precision of the different commercially available troponin assays vary considerably. These differences are related to a lack of standardization, the use of different monoclonal antibodies, the presence of modified TnI and TnT in the serum, and variations in antibody cross-reactivity to the various detectable forms of TnI that result from its degradation.
Only one manufacturer produces the TnT assay, and its 99th percentile cutoffs and the 10% CV are well established. However, up to 20-fold variation has occurred in results obtained with the multitude of commercial TnI assays currently available, each with their own 99th percentile upper reference limits and 10% CV levels.
In the GUSTO IV study, a relatively insensitive point-of-care TnI assay was used to screen patients for study eligibility. In a subsequent study, the blood samples were reanalyzed using the 99th percentile cutoff of a far more sensitive central laboratory TnT assay. The more sensitive 99th percentile cutoff of this TnT assay identified an additional 96 (28%) of 337 patients with a positive TnT result but negative point-of-care TnI; these patients had higher rates of death or MI at 30 days.
In a similar reanalysis of the TACTICS-TIMI 18 trial, 3 different TnI cutoffs were compared on 1821 patients to evaluate the 30-day risk of death or MI: the 99th percentile, 10% CV, and the World Health Organization (WHO) acute MI cutoffs. (The WHO cutoffs define acute MI using CK-MB and report troponin levels as either a higher “acute MI level” or a lower “intermediate level” that is correlated with “leak” or “minor myocardial injury.”)
Using the 10% CV cutoff identified, an additional 12% more cases were identified relative to the WHO acute MI cutoff. The 99th percentile cutoff identified an additional 10% of cases relative to the 10% CV cutoff, as well as a 22% increase in the number of cases over the WHO acute MI cutoff. Nevertheless, the odds ratios for the adverse cardiac event rates of death or MI at 30 days were similar for all 3 cutoffs, suggesting that the lower cutoffs detected more patients with cardiovascular risk without sacrificing specificity.
Creatine Kinase–MB
Prior to the introduction of cardiac troponins, the biochemical marker of choice for the diagnosis of acute MI was the CK-MB isoenzyme. The criterion most commonly used for the diagnosis of acute MI was 2 serial elevations above the diagnostic cutoff level or a single result more than twice the upper limit of normal. Although CK-MB is more concentrated in the myocardium, it also exists in skeletal muscle and false-positive elevations occur in a number of clinical settings, including trauma, heavy exertion, and myopathy.
CK-MB first appears 4-6 hours after symptom onset, peaks at 24 hours, and returns to normal in 48-72 hours. Its value in the early and late (>72 h) diagnosis of acute MI is limited. However, its release kinetics can assist in diagnosing reinfarction if levels rise after initially declining following acute MI.
In the CRUSADE registry, a review of almost 30,000 patients revealed that discordant troponin and CK-MB results occurred in 28% of patients. However, patients who were troponin negative but CK-MB positive had in-hospital mortality rates that were not significantly increased from patients who were negative for both biomarkers.
Similarly, in a report of more than 10,000 patients with ACS from the multicenter GRACE registry, in-hospital mortality was highest when both troponin and CK-MB were positive, intermediate in troponin-positive/CK-MB-negative patients, and lowest in patients in whom both markers were negative and in those who were troponin-negative/CK-MB-positive. [34] Thus, an isolated CK-MB elevation has limited prognostic value in patients with a non-ST elevation ACS.
CK-MB/CK relative index
The relative index calculated by the ratio of CK-MB (mass) to total CK can assist in differentiating false-positive elevations of CK-MB arising from skeletal muscle. A ratio of less than 3 is consistent with a skeletal muscle source, while ratios greater than 5 are indicative of a cardiac source. Ratios between 3 and 5 represent a gray zone. No definitive diagnosis can be established without serial determinations to detect a rise.
The CK-MB/CK relative index was introduced to improve the specificity of CK-MB elevation for myocardial infarction. However, sensitivity for acute MI falls when concurrent cardiac injury and skeletal muscle injury is present. In an ED-based study to evaluate the CK-MB relative index compared with the absolute CK-MB, specificity was increased, but with a loss of sensitivity.
The CK-MB/CK relative index is useful if patients have only an MI or only skeletal muscle injury, but not if they have both. Therefore, in the combined setting of acute MI and skeletal muscle injury (rhabdomyolysis, heavy exercise, polymyositis), the fall in sensitivity is significant.
Note that the diagnosis of acute MI must not be based on an elevated relative index alone, because the relative index may be elevated in clinical settings when either the total CK or the CK-MB is within normal limits. The relative index is only clinically useful when both the total CK and the CK-MB levels are increased.
Source emedicine.com
Duc Tin Surgical Clinic
Tin tức liên quan
Performance diagnostique de l’interféron gamma dans l’identification de l’origine tuberculeuse des pleurésies exsudatives
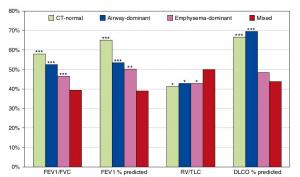
A Mixed Phenotype of Airway Wall Thickening and Emphysema Is Associated with Dyspnea and Hospitalization for Chronic Obstructive Pulmonary Disease.
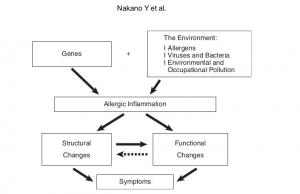
Radiological Approach to Asthma and COPD-The Role of Computed Tomography.

Significant annual cost savings found with UrgoStart in UK and Germany
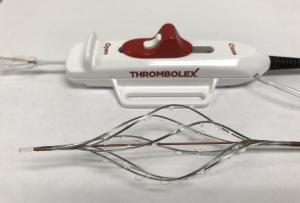
Thrombolex announces 510(k) clearance of Bashir catheter systems for thromboembolic disorders
Phone: (028) 3981 2678
Mobile: 0903 839 878 - 0909 384 389