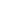The PASCAL repair system (Edwards Lifesciences, Irvine, CA, USA) is a novel leaflet repair therapy. The implant uses clasps and paddles that gently grasp leaflets to facilitate coaptation. The device is implanted via transseptal approach and places a spacer between the valve leaflets to fill the regurgitant orifice.
The CLASP study is a multicentre, multinational, prospective, single-arm study that evaluated the use of the PASCAL repair system for the management of mitral regurgitation (both degenerative and functional). The results from the CLASP study show that the PASCAL repair system is associated with a very important and significant reduction in mitral regurgitation (MR) with 86% of patients having residual MR grade of ≤1+, and 98% of patients with residual MR grade of ≤2+ at 30 days.1
Ulrich Schäfer (Catholic Marienhospital Hamburg, Hamburg, Germany), a CLASP study investigator, explains that CLASP was “a safety and efficacy trial” to “prove the concept” behind the device.
The CLASP study investigators, Lim DS et al, report that the PASCAL repair system paddles “are designed to minimise stress concentration on the native leaflets” and the spacer is “intended to fill the regurgitant orifice area to reduce MR”.1 For Schäfer, these features make the PASCAL repair system “very interesting and innovative” because they are different from those seen with other transcatheter mitral valve repair therapies. He notes that the clasps on the system can be independently adjusted, which enables “a very sophisticated approach to leaflet capture”.
Volker Rudolph (Heart and Diabetes Center, University Clinic, Bad Oeynhausen, Germany) also uses the PASCAL repair system at his centre and, like Schäfer, believes that its unique features may provide several advantages. He comments: “With mitral valve repair, whatever technique you use, you want to achieve maximal leaflet coaptation without impeding forward flow through the valve. I think the PASCAL repair system allows you to reach that goal very efficiently.” In particular, the less rigid, broad nitinol paddles and the central spacer probably help to place less stress on the leaflets while the spacer may reduce the risk of creating an artificial stenosis. Rudolph explains that when you implant a device to repair the mitral valve, you pull the anterior and posterior leaflets together. “If you do this very efficiently, you may create a stenosis which causes the leaflets not to open effectively. However, with a spacer, you are not pulling on the leaflets as much. Therefore, you have more mobility for the leaflets and more residual orifice area. You reduce the leak but maintain movement,” he says.
“The other major aspect that helps optimise coaptation is the separate manoeuvrability of the clasps. This means you can correct the grasping position for the anterior leaflet independent of the posterior leaflet,” Rudolph explains. He adds: “The morphologies of the mitral valve can sometimes be challenging and the forces counteracting on coaptation can only partly be identified from available imaging techniques. Therefore, the ability to do a minor correction of the device by re-grasping just one leaflet with the pliable nitinol paddles is a major advancement that allows an easier optimisation of leaflet coaptation, which often has a significant impact on the procedural result.”
Source CardiovascularNews
Duc Tin Clinic
Tin tức liên quan
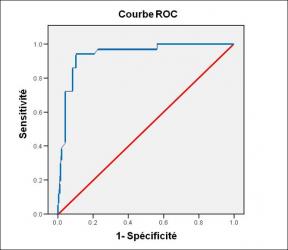
Performance diagnostique de l’interféron gamma dans l’identification de l’origine tuberculeuse des pleurésies exsudatives
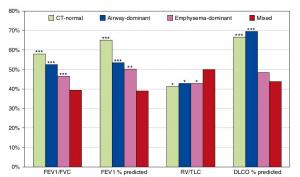
A Mixed Phenotype of Airway Wall Thickening and Emphysema Is Associated with Dyspnea and Hospitalization for Chronic Obstructive Pulmonary Disease.
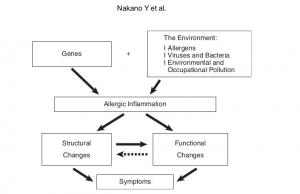
Radiological Approach to Asthma and COPD-The Role of Computed Tomography.

Significant annual cost savings found with UrgoStart in UK and Germany
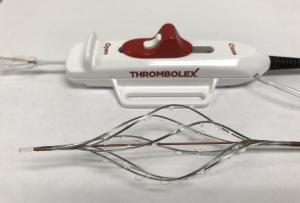
Thrombolex announces 510(k) clearance of Bashir catheter systems for thromboembolic disorders
Phone: (028) 3981 2678
Mobile: 0903 839 878 - 0909 384 389