Data from the CLASP study
The CLASP study enrolled 62 patients with MR grade 3+ or 4+ (56% functional, 36% degenerative, and 8% with mixed aetiology). The patients had a mean age of 76.5 years and 51.6% were in New York Heart Association (NYHA) class III or IV.1
At 30 days, of those with a successful implantation (59 patients), 98% of patients had an improvement in MR by one grade or more. This meant that 98% of patients had MR grade ≤2+ and 86% of patients had MR grade ≤1+ (significantly reduced compared with baseline levels, p<0.0001; Figure 1). Schäfer calls these results “remarkable”, noting that the reduction in MR is “very profound”. Another study with MitraClip, COAPT, which only included patients with functional MR, showed 92.7% of patients had MR grade ≤2+ and 72.9% had MR grade ≤1+ at 30 days.1,2 Additionally, Schäfer observes, COAPT was a trial with procedures performed by operators with extensive device experience, whereas CLASP was a trial in which the study investigators had less experience with the device by the nature of the PASCAL repair system being a novel implant. “The COAPT study showed the best-ever published data regarding the success of reducing MR. Now the CLASP study shows very important reductions in MR. I think that these findings of CLASP are very interesting.”
Importantly, successful implantation was achieved in 95% of patients, with an average of 1.5 devices implanted per patient. Furthermore, the 30-day all-cause mortality rate in CLASP was low (1.6%; one patient). The death was procedural, as a consequence of a vascular complication at the closure of the femoral access, rather than of the device itself. According to Schäfer, any mortality rate below 5% in a high-risk patient population such as that of the CLASP study is low. He notes all patients, prior to enrolment, were assessed by a multidisciplinary heart team and deemed to be at high risk for surgery.
At the 2019 Transcatheter Valve Therapeutics (TVT) meeting (12–15 June, Chicago, USA), Scott Lim (University of Virginia Health System Hospital, Charlottesville, USA) reported, on behalf of the CLASP study investigators, the six-month results of the CLASP study.3 These showed that the significant reductions in MR seen at 30 days were sustained: at six months 98% of patients had MR grade ≤2+ and 81% had MR grade ≤1+ (Figure 1). Additionally, 88% of patients were in NYHA class I or II and 46% of patients in NYHA class I (these figures were 85% and 37%, respectively, at 30 days) thus showing further improvements; and a significant difference compared with baseline levels (p<0.0001).
Importantly, mean transmitral valve gradient at 30 days was 4mmHg (p<0.0001 vs. baseline levels) and this result was also sustained at six months (Figure 2), which shows that the PASCAL repair system facilitates leaflet coaptation and wide diastolic openings. Importantly, these results were obtained with 1.5 average devices per patient. Rudolph says: “There is a critical cut-off point when reducing residual flow and, once passed, you are potentially creating a barrier to forward flow—meaning that the heart cannot fill properly with blood. You would expect that if you had a wider device or two devices, if you took more of the leaflets, the risk of such a barrier would be much more likely. With the PASCAL repair system, I think this risk is probably mitigated by the spacer and how it facilitates leaflet coaptation and wider diastolic openings.”
Summing up the data for the PASCAL repair system, Schäfer states: “The outcomes are very convincing. For me, the most striking finding was the very significant reduction in mitral regurgitation.”
Although not explored in the CLASP study, the width of the PASCAL implant may enable operators to only use one device in most cases, and in certain patients with degenerative MR this could be particularly advantageous. Rudolph explains: “In some cases of degenerative mitral regurgitation, getting to all of the diseased parts of the valve can be very challenging. Just imagine if the leaflet is not attached to the chordae in the ventricle, then—in systole—it flips towards the atrial side and it becomes a flail leaflet. Therefore, if it is very wide and you have a narrow device, you might grasp some of it but still have parts that prolapse into the left atrium. But if you have a wider device, achieving maximal coaptation and wider diastolic openings with one device will be much easier.”
In their commentary on the CLASP study, Praz et al write: “The advent of the PASCAL repair system is a welcome addition to the armamentarium of transcatheter mitral valve devices. The early experience attests to the feasibility of the procedure, and further studies will be instrumental to define the appropriate use and indication for this novel device.”
Source CardiovascularNews
Duc Tin Clinic
Tin tức liên quan
Performance diagnostique de l’interféron gamma dans l’identification de l’origine tuberculeuse des pleurésies exsudatives
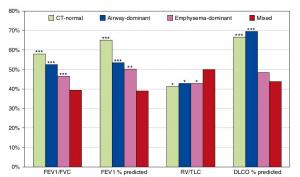
A Mixed Phenotype of Airway Wall Thickening and Emphysema Is Associated with Dyspnea and Hospitalization for Chronic Obstructive Pulmonary Disease.
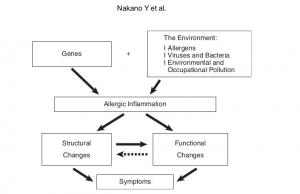
Radiological Approach to Asthma and COPD-The Role of Computed Tomography.

Significant annual cost savings found with UrgoStart in UK and Germany
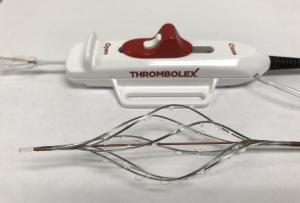
Thrombolex announces 510(k) clearance of Bashir catheter systems for thromboembolic disorders
Phone: (028) 3981 2678
Mobile: 0903 839 878 - 0909 384 389