A systematic review and meta-analysis has demonstrated that patients undergoing carotid interventions after thrombolysis have a higher risk of periprocedural hazards, compared with those patients who did not have prior thrombolysis. Authors Stavros K Kakkos (University Hospital of Patras, Patras, Greece) and colleagues report their findings in an article published online in the European Journal of Vascular and Endovascular Surgery (EJVES).
“Patients undergoing carotid endarterectomy (CEA) or carotid artery stenting (CAS) after thrombolytic therapy have a higher risk of periprocedural stroke and death, compared with patients undergoing CEA or CAS without prior thrombolytic therapy,” the authors write. However, they note that the difference was statistically significant only for CAS. In regards to other hazards, Kakkos et al note that there was also a higher risk of periprocedural intracranial haemorrhage (ICH) and local haematoma in patients undergoing carotid interventions after thrombolysis.
One of the findings that Kakkos and colleagues state is “of most practical importance” is that periprocedural risks of stroke and death appeared to be higher if CEA was performed in the first few days after thrombolysis. This inverse relationship between timing to CEA and periprocedural stroke/death “mandates careful patient selection and suggests that it may be safer to defer CEA for six to seven days after thrombolytic therapy,” they posit in EJVES.
Using the Medline, Scopus, and Cochrane databases, Kakkos et al identified 25 studies involving patients who underwent either CEA or CAS after thrombolytic therapy to include in their systematic review and meta-analysis. There were a total of 147,810 patients in these 25 studies, 2,557 of whom underwent either CEA (n=2,076) or CAS (n=481) following thrombolytic therapy.
After CEA, the authors report that the pooled periprocedural stroke/death rate was 5.2% (95% confidence interval [CI], 3.3–7.5) and intracranial haemorrhage was 2.4% (95% CI, 1.7–5.6). After CAS, they relay, the pooled perioperative procedural stroke/death rate was 14.9% (95% CI, 11.9–18.2) and ICH was 5.5% (95% CI, 3.7–7.7).
In case control studies comparing CAS outcomes in patients receiving thrombolytic therapy versus no thrombolytic therapy, the authors communicate that periprocedural stroke/death was significantly higher after thrombolytic therapy (5.2% vs. 1.5%; odds ratio [OR] 8.49; 95% CI, 2.12–33.95), as was ICH (5.4% vs. 0.7%; OR, 7.48; 95% CI, 4.69–11.92).
Kakkos and colleagues also detail that meta-regression analysis demonstrated an inverse association between the time interval from intravenous thrombolytic therapy to undergoing CEA and the risk of periprocedural stroke/death (p=0.032). “Perioperative stroke/death was 13% when CEA was performed three days after thrombolytic therapy and 10.6% when performed four days after thrombolytic therapy, with the risk reducing to within the currently accepted 6% threshold after six–seven days had elapsed,” they write in EJVES, communicating the results of their analysis.
The authors acknowledge that a “major limitation” of their systematic review and meta-analysis is that there were no randomised controlled trials to inform clinical practice. “This is especially relevant regarding stratifying procedural risks in stroke patients who do not have any computed tomography (CT)/magnetic resonance imaging (MRI) evidence of infarction post-thrombolytic therapy and for evaluating the benefits of deferring CEA for six-seven days,” they comment.
In addition, Kakkos et al recognise that case control studies have inherent biases because of study design, so that patients receiving thrombolysis “may have had more severe strokes”. This, they note, could explain the worse outcomes observed in their systematic review.
Finally, the researchers state that varying exclusion criteria, timing, and mode of thrombolytic therapy administration, may have caused heterogeneity, and “should be explored in future studies”.
Source VascularNews
Duc Tin Clinic
Tin tức liên quan
Performance diagnostique de l’interféron gamma dans l’identification de l’origine tuberculeuse des pleurésies exsudatives
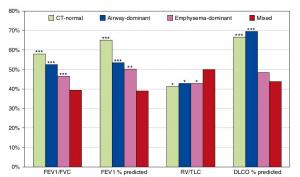
A Mixed Phenotype of Airway Wall Thickening and Emphysema Is Associated with Dyspnea and Hospitalization for Chronic Obstructive Pulmonary Disease.
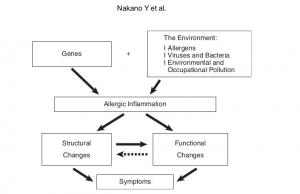
Radiological Approach to Asthma and COPD-The Role of Computed Tomography.

Significant annual cost savings found with UrgoStart in UK and Germany
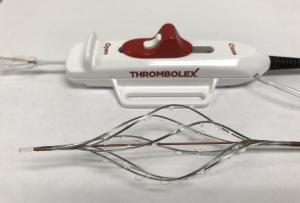
Thrombolex announces 510(k) clearance of Bashir catheter systems for thromboembolic disorders
Phone: (028) 3981 2678
Mobile: 0903 839 878 - 0909 384 389